Summary
A hydrocele is a painless collection of fluid around the testicle, causing swelling in the scrotum. It is common in newborn boys and usually resolves on its own within the first year of life. In rare cases, a similar condition can occur in females along the canal of Nuck.
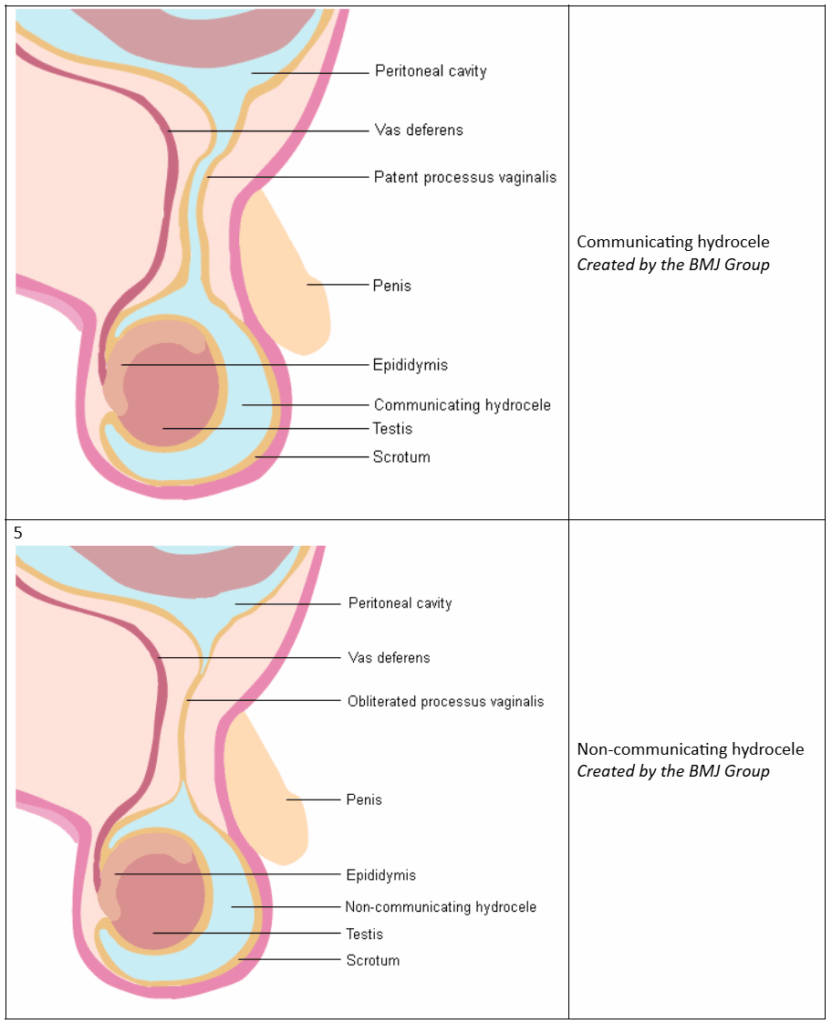
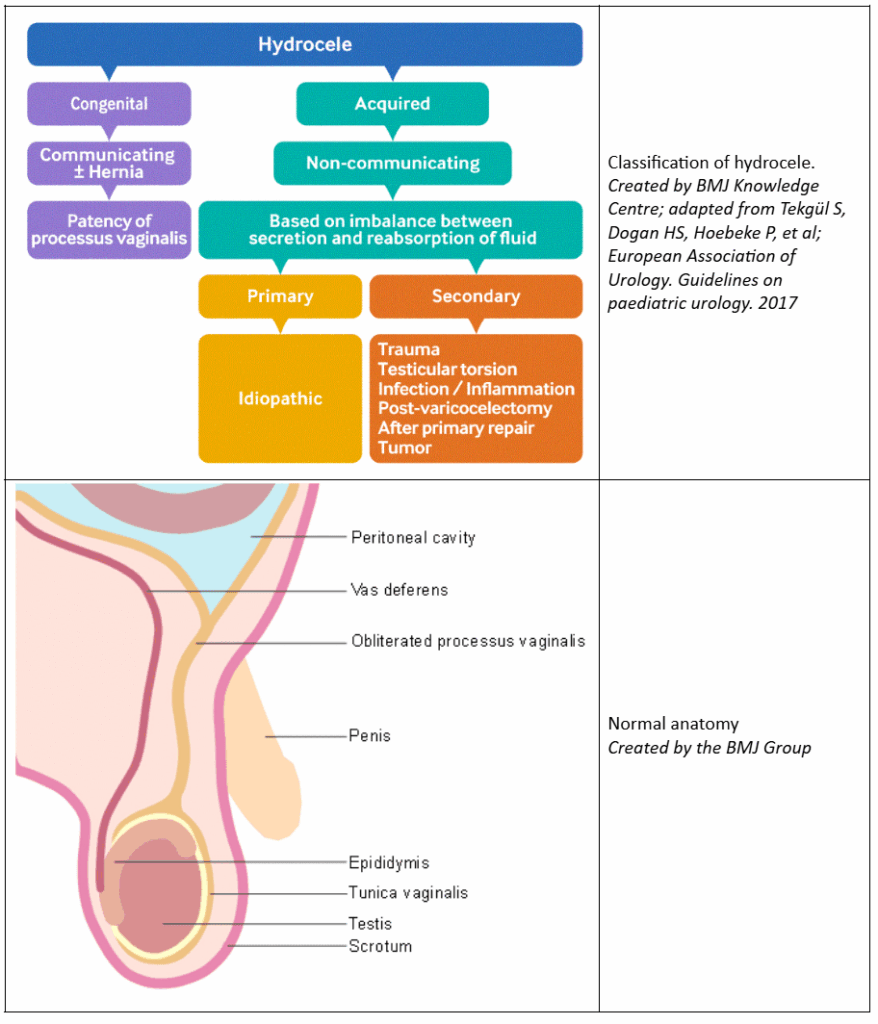
There are two types of hydroceles:
- Communicating hydrocele: A small opening between the abdomen and scrotum allows fluid to move in and out, sometimes causing the swelling to change in size.
Non-communicating hydrocele: The fluid is trapped in the scrotum without connection to the abdomen, typically resolving without treatment.
Diagnosis and When to Seek Help
Parents should consult a doctor if their child has:
- A painless swelling in one or both sides of the scrotum
- A scrotum that appears larger at different times of the day (suggesting a communicating hydrocele)
- Persistent swelling beyond 12–18 months of age
Doctors can usually diagnose a hydrocele with a physical exam. In some cases, transillumination (shining a light through the scrotum) or an ultrasound may be used to confirm the diagnosis and rule out other conditions.
Management
- Observation: Most hydroceles in infants resolve on their own by 12 to 18 months without any treatment.
- Surgery: If the hydrocele persists beyond 18 months, causes discomfort, or is associated with an inguinal hernia, a surgical procedure called hydrocelectomy may be needed. This is a minor outpatient procedure.
Follow-Up and Monitoring
After diagnosis, regular follow-ups may be recommended to monitor the hydrocele. If surgery is required, children typically recover quickly with minimal discomfort.
If you notice persistent or changing swelling in your child’s scrotum, consult a doctor to determine the best course of action.
History and Exam
Key diagnostic factor
- Presence of risk factors
- Scrotal mass
- Transillumination
- Enlargement of scrotal mass following activity
Other diagnostic factors
- Male sex
- Prematurity and low birth weight
- Infants <6 months of age
- Infants whose testes descend relatively late
Diagnostic Investigations
1st investigations to order
- Clinical diagnosis
Investigations to consider
- Ultrasound

Book an Appointment
Other Related Conditions
congenital hernias
removal of lumps and lesions

pilonidal sinuses
in-grown toenails
acute scrotal pain

