Summary
Food allergies occur when the body’s immune system mistakenly reacts to harmless proteins in food as though they are harmful. Common allergens include peanuts, tree nuts, milk, eggs, fish, shellfish, wheat, and soya. Most allergic reactions occur within 20 minutes of eating, and nearly always within two hours.
Symptoms can range from mild reactions like itching and skin rashes to severe symptoms such as difficulty breathing, swelling, and even life-threatening anaphylaxis. Anaphylaxis requires immediate treatment with epinephrine (adrenaline) to prevent serious complications. For less severe reactions, treatment may include removing the allergen and using antihistamines.
Diagnosis and When to Seek Help
If your child experiences any of the following symptoms after eating certain foods, seek medical attention:
- Itching or skin rashes
- Swelling of the lips, face, or throat
- Breathing difficulties (wheezing, shortness of breath)
- Dizziness or fainting
Abdominal pain, vomiting, or diarrhea
If anaphylaxis (severe allergic reaction) occurs, immediate injection of epinephrine and urgent medical care are required.
Management
Managing food allergies involves a combination of prevention, emergency preparedness, and long-term management:
- Avoidance of the triggering food is the primary preventive measure.
- Epinephrine (adrenaline) auto-injectors should be kept at all times, and the child should be taught how to use it correctly.
- Emergency plan: Parents should ensure their child has access to medical identification jewellery and is well-prepared to recognize and react to symptoms of an allergic reaction.
- Other treatments: For less severe reactions, antihistamines may help alleviate symptoms.
Follow-Up and Monitoring
Regular follow-up visits with an allergist are essential to monitor the allergy and adjust the treatment plan if necessary. Parents should continue to be vigilant about potential exposures to allergens and ensure their child understands how to avoid triggers and use the epinephrine auto-injector.
Food allergies can be life-threatening, so a comprehensive approach to management—including prevention, preparation, and quick response—is critical for keeping your child safe.
History and Exam
Key diagnostic factors
- Presence of risk factors
- Milk, egg, nut, fish, shellfish, wheat, or soya ingestion
- Reproducible symptoms
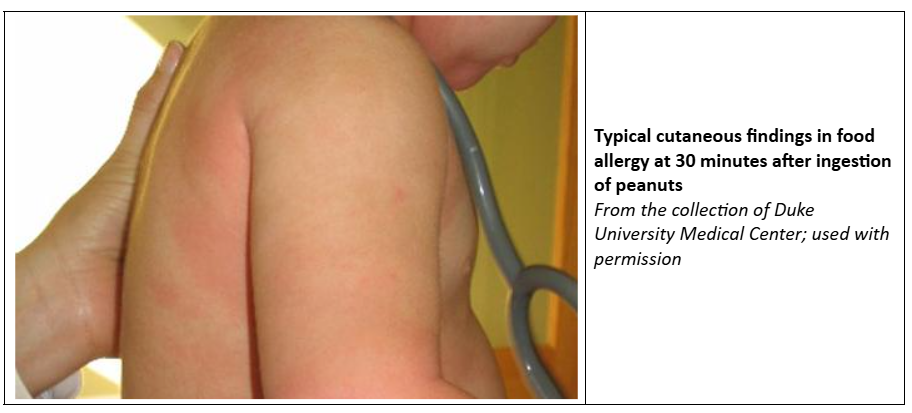
- Flushing, urticaria, or angio-oedema of the skin
Other diagnostic factors
- Tachycardia or bradycardia
- Reaction exacerbated by exercise or exertion
- Alcohol or medication ingestion before reaction
- Cardiac arrhythmia
Risk factors
- Family history of food allergy
- Atopic dermatitis
- Newborn
- Perinatal peanut oil exposure
Diagnostic Investigations
1st investigations to order
- In vitro IgE-specific immunoassay
- Skin prick testin
Investigations to consider
- Food challenges
- Component-resolved diagnostics
Emerging tests
- Atopy patch testin

