Summary
Anaphylaxis is a severe and potentially life-threatening allergic reaction that occurs suddenly after exposure to an allergen. It can affect breathing, circulation, and the airway, sometimes without noticeable skin changes. Common signs include skin rash, wheezing, difficulty breathing, and low blood pressure.
Immediate treatment with intramuscular adrenaline (epinephrine) is critical and can save lives. Allergy testing can help identify triggers and prevent future episodes.
Diagnosis and When to Seek Help
Anaphylaxis is diagnosed based on symptoms and the rapid onset of a severe allergic reaction. Parents should seek emergency medical help if their child experiences:
- Difficulty breathing, wheezing, or a hoarse voice.
- Swelling of the face, lips, tongue, or throat.
- Dizziness, confusion, or fainting.
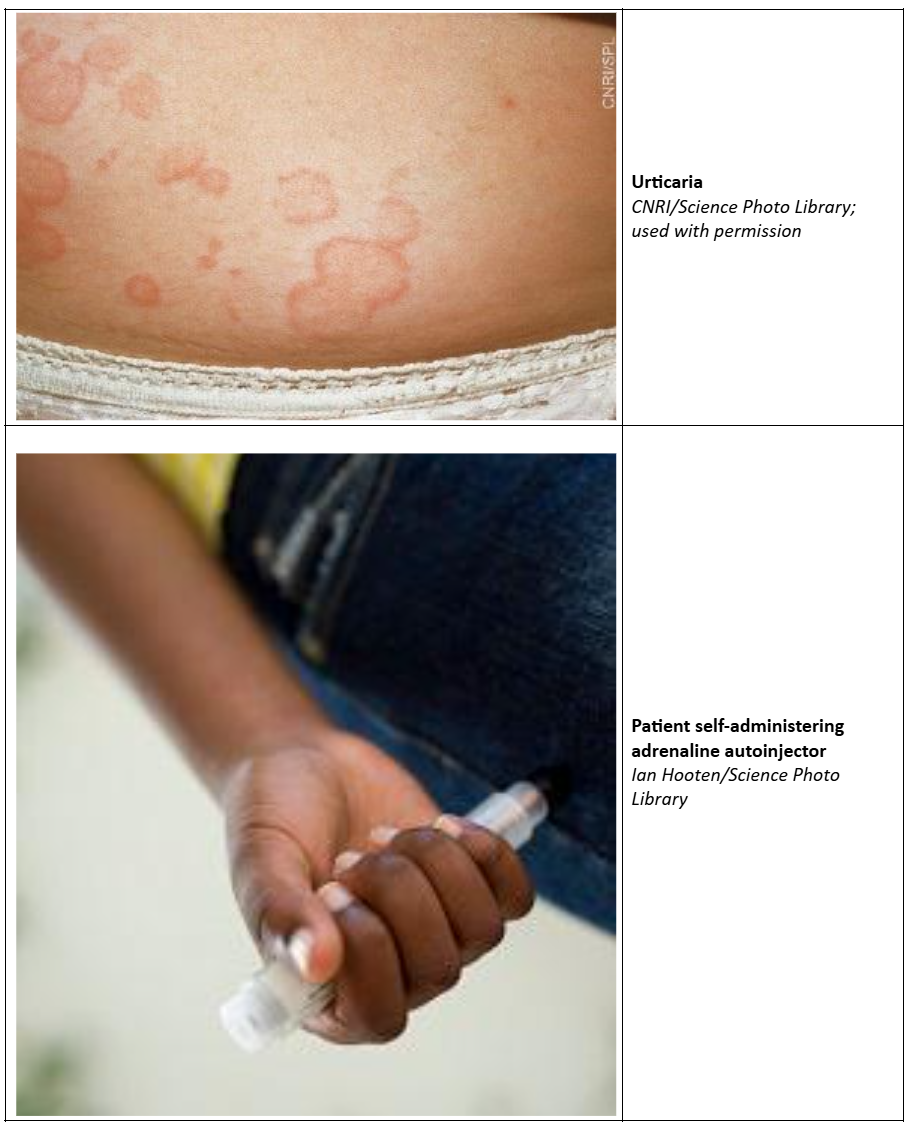
- A widespread rash with severe itching.
- A known exposure to an allergen followed by rapid symptom onset.
Management
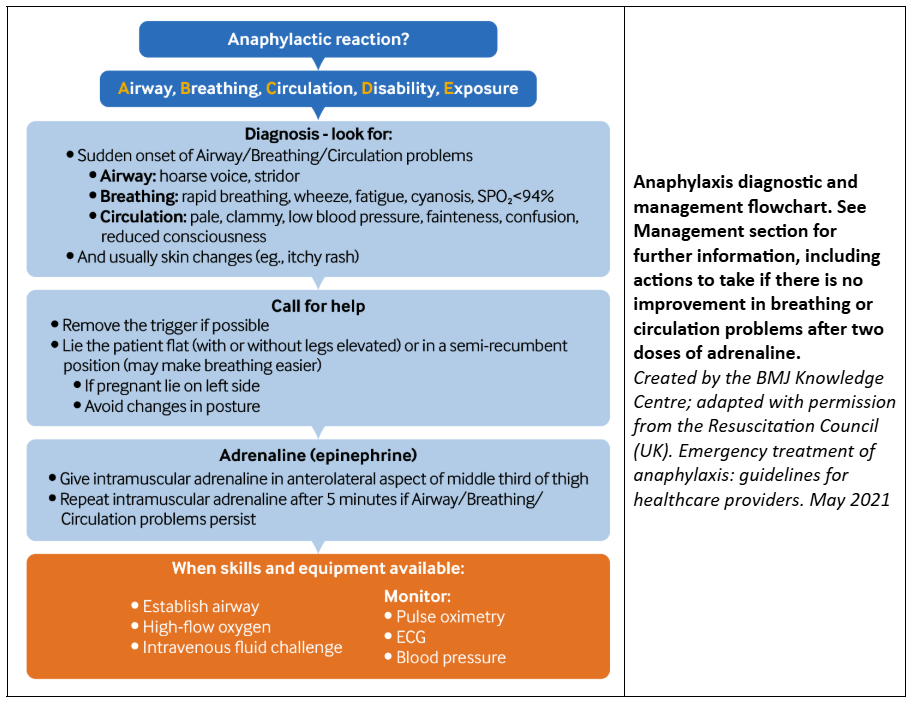
Managing anaphylaxis requires immediate action and long-term planning. Treatment options include:
- Emergency Treatment:
- Intramuscular adrenaline (epinephrine): The first-line treatment for stopping anaphylaxis. Parents should always carry an adrenaline auto-injector if their child has a known severe allergy.
- Calling Emergency Services: Anaphylaxis is a medical emergency requiring immediate care.
- Lying the Child Flat: If the child is dizzy or faint, keeping them flat can help maintain circulation. If breathing is difficult, sitting upright may be better.
- Long-Term Management:
- Avoidance of Triggers: Identifying and avoiding known allergens such as specific foods, insect stings, or medications is essential.
- Allergy Testing: Helps confirm the specific triggers of anaphylaxis.
- Adrenaline Auto-Injector Training: Parents, caregivers, and school staff should be trained to use an auto-injector in case of an emergency.
- Medical Alert Identification: Wearing a medical bracelet or carrying an allergy card can help in emergencies.
Follow-Up and Monitoring
Ongoing care is essential for children at risk of anaphylaxis. Parents should:
- Ensure their child has access to an adrenaline auto-injector at all times.
- Have a written emergency action plan provided by their doctor.
- Schedule regular follow-ups with an allergist to monitor the condition.
- Educate caregivers, teachers, and family members on recognizing and responding to anaphylaxis.
With proper emergency preparedness and avoidance strategies, children at risk of anaphylaxis can lead safe and healthy lives.
History and Exam
Key diagnostic factors
- acute onset
- airway swelling (angio-oedema)
- inspiratory stridor and hoarse voice
- shortness of breath
Other diagnostic factors
- risk factors
- nausea, vomiting, diarrhoea, and incontinence
- abdominal cramps and pain
- agitation, anxiety, and a sense of impending doom (angor animi)
Risk factors
- adult age: food, insect venom and medicine-related
- <30 years old: food-associated, exercise-induced
- female sex
- atopy/asthma
Diagnostic Investigations
1st investigations to order
- mast cell tryptase
- 12-lead ECG
- blood gases
- urea and electrolytes
Investigations to consider
- chest x-ray

