Summary
Urticaria, commonly known as hives, is a skin condition that causes red, itchy, and swollen patches (welts) on the skin. These welts can vary in size and shape and may appear anywhere on the body. They usually last for a few hours but can persist for up to 24 hours before fading. Hives can be triggered by allergic reactions, infections, heat, stress, or unknown causes.
Diagnosis and When to Seek Help
Hives are diagnosed based on their appearance and symptoms. Parents should seek medical advice if:
- The hives last for more than six weeks (chronic urticaria).
- The child experiences swelling of the lips, tongue, or throat (angioedema).
- There are signs of a severe allergic reaction, such as difficulty breathing or dizziness (seek emergency care immediately).
- The hives keep coming back without an obvious cause.
Management
Treatment depends on the cause and severity of the hives:
- Mild Cases: Over-the-counter antihistamines can help reduce itching and swelling.
- Severe or Persistent Cases: A doctor may prescribe stronger antihistamines or other medications to control symptoms.
- Identifying Triggers: If a specific allergen or irritant is suspected, avoiding it can help prevent future outbreaks.
- Chronic Urticaria: If hives last for more than six weeks, further testing may be needed to identify potential underlying causes.
Follow-Up and Monitoring
- Keep a record of possible triggers, such as foods, medications, or environmental factors.
- Ensure your child takes prescribed medications as directed.
- Follow up with a doctor if hives persist or worsen.
With the right management, most cases of urticaria can be controlled, allowing children to remain comfortable and active.

History and Exam
Key diagnostic factors
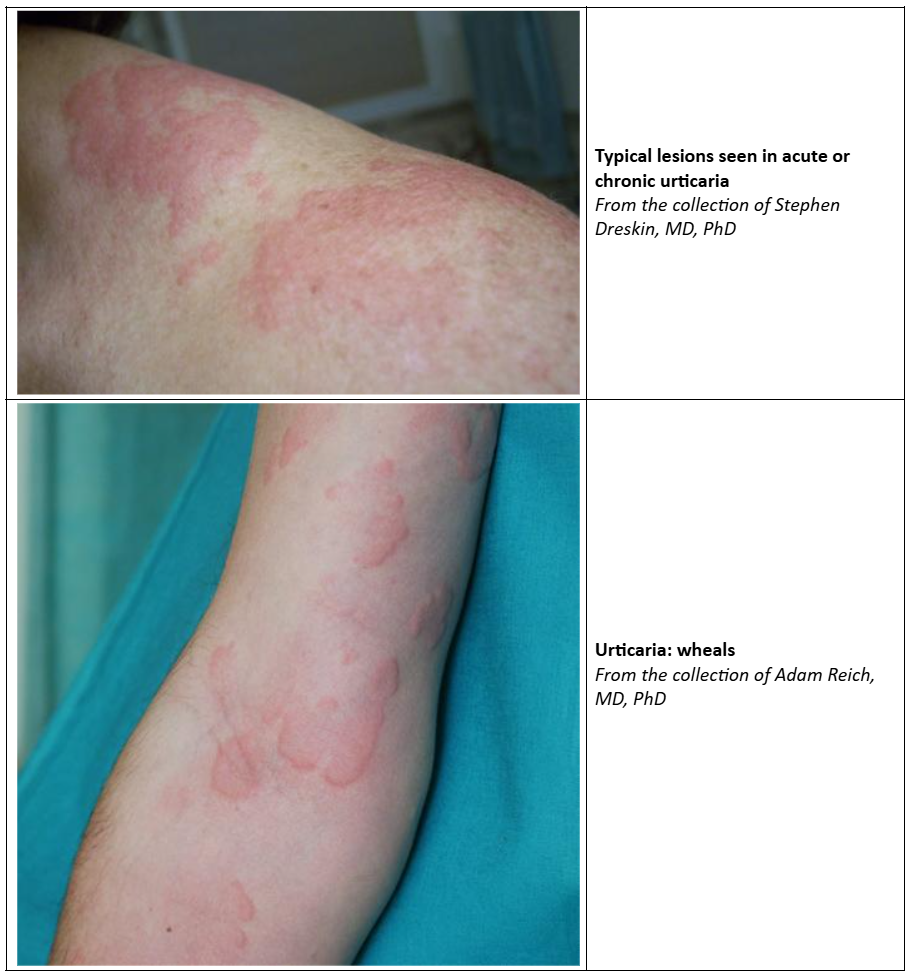
- Erythematous oedematous lesions
- Pruritus
- Resolution within 24 hours
- Swelling of face, tongue, or lips
Other diagnostic factors
- Blanching lesions
- stridor
Risk factors
- positive family history
- female sex
- exposure to drug trigger
- exposure to food trigger
Diagnostic Investigations
1st investigations to order
- FBC with differential
- Erythrocyte sedimentation rate (ESR)
- CRP
- C4 level
Investigations to consider
- Thyroid-stimulating hormone (TSH)
- Antinuclear antibodies (ANA)
- Skin prick testing
- Allergen avoidance diet

